West Coast Retina
Case of the Month
December, 2011
Presented by Sandeep Randhawa, MD
A 49-year-old woman referred for hyperpigmented fundus lesions in both eyes.

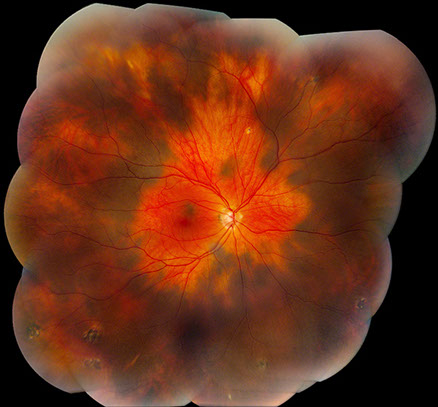
A
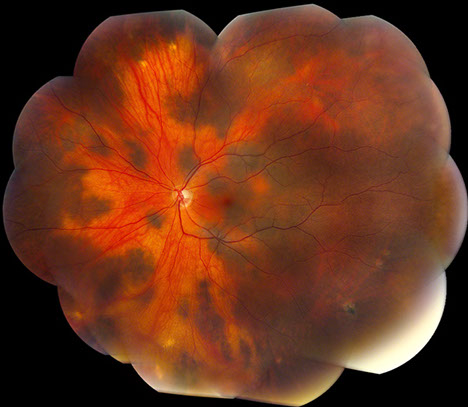
B
Figures 1A and B: Fundus photograph montages of the right and left eye. Note the extensive, bilateral increase pigmentation in each eye. It appears patchy and isolated in some areas, but in most areas, the pigmentation is increased diffusely.
Case History
A 49-year-old asymptomatic Latina woman was referred for evaluation of bilateral, diffuse hyperpigmented fundus lesions discovered on a routine eye examination. Best-corrected visual acuity was 20/20 in each eye and her intraocular pressures were normal bilaterally. There was no vitiligo or hyperpigmentation of the periocular skin, conjunctiva, episclera or sclera. Gonioscopy and slit lamp examination of the anterior segment were normal bilaterally. Dilated fundus examination revealed extensive hyperpigmented choroidal lesions diffusely distributed in a circumferential pattern (Figure 1A and B). Larger choroidal vessels were visible in some areas, and several isolated patches of increased pigmentation were noted most prominently in the left eye where they also involved the posterior pole. The lesions were not thickened and no subretinal fluid was present. A few scattered punched out chorioretinal scars were present in the periphery. Past medical, surgical, social and family histories were non-contributory.
What is your Diagnosis?
Differential Diagnosis
The differential diagnosis includes disorders that are associated with both increased and decreased choroidal pigmentation. Increased choroidal pigmentation, as observed in our patient can be seen with: ocular and oculodermal melanocytosis, diffuse choroidal melanoma, and bilateral diffuse uveal melanocytic proliferation. Important findings in our case included the absence of choroidal thickening, lack of subretinal fluid, normal vision, no associated hypo- or hyperpigmentation of the skin or sclera and no systemic malignancy which collectively exclude these diagnoses.
Significant differences in choroidal hyperpigmentation can also be secondary to hypopigmentation which maybe more striking in pigmented races. Such patients tend to have findings of cutaneous vitiligo.1,2 Up to 40% of patients with cutaneous vitiligo may have some hypopigmentation of the choroid.3 However, our patient did not have any evidence of vitiligo. Choroidal hypopigmentation may also be secondary to prior posterior uveitis as in Vogt-Koyanagi-Harada syndrome (‘sunset-glow’ fundus).4 Our patient did not have any history of uveitis.
Additionally, degenerative changes of the posterior pole secondary to posterior staphyloma in pathologic myopia can leave a relative hypopigmented posterior pole in comparison to the peripheral fundus.
Flat melanocytic choroidal hyperpigmentation in the absence of any hyperpigmentation of the sclera or skin has been described and termed isolated choroidal melanocytosis. Our patient was diagnosed with bilateral isolated choroidal melanocytosis.
Discussion
Bilateral isolated choroidal melanocytosis is an uncommon disorder characterized by the presence of flat melanocytic hyperpigmentation of the choroid in the absence of hypo- or hyperpigmentation of the skin or sclera.
Augsberger et al previously reported a series with unilateral involvement that was also limited to less than three clock-hours of involvement.5 These authors also observed feathered margins and sparing of large choroidal vessels. Kovoor et al reported an Asian Indian woman with bilateral isolated choroidal melanocytosis with involvement of the posterior pole and relative sparing of the periphery.6 Fine and Yannuzzi described a case of bilateral isolated choroidal melanocytosis with twelve-clock hours of circumferential involvement, a pattern very similar to our case.7
The relative sparing of the large choroidal vessel may localize the depth of the hyperpigmentation to the choroidal stroma, the location of larger choroidal vessels and melanocytes. Patients with ocular or oculodermal melanocytosis (Nevus of Ota) have up to a 35-fold increased risk of developing uveal melanoma. It is estimated that one in 400 Caucasian patients with ocular melanocytosis followed for life will develop uveal melanoma.8 Our patient was Latina and so has a lower risk. There have been no reports describing the histology of hyperpigmentation in isolated choroidal melanocytosis. An annual follow up is recommended.
Take Home Points
- Ophthalmologists should be aware that isolated choroidal melanocytosis can present bilaterally and with diffuse circumferential involvement.
- Lesions may involve either the posterior pole or the periphery.
- Isolated choroidal melanocytosis can be differentiated from choroidal vitiligo by an absence of cutaneous findings
- An annual follow-up examination is recommended for patients with isolated choroidal melanocytosis, despite the generally benign course.
Want to Subscribe to Case of the Month?
References
- Ciardella AP, Horsley M. Hypopigmentary fundus changes seen with cutaneous vitiligo. Arch Ophthalmol 2007;125:576.
- Shields CL, Ramasubramanian A, Kunz WB, Aggarwal E, Shields JA. Choroidal vitiligo masquerading as large choroidal nevus: a report of four cases Ophthamology. 2010 Jan;117(1):109-113.
- Albert DM, Nordlund JJ, Lerner AB. Ocular abnormalities occurring with vitiligo. Ophthalmology 1979; 86:1145-1160.
- Keino H, Goto H, Usui M. Sunset glow fundus in Vogt-Koyanagi-Harada disease with or without chronic ocular inflammation. Graefes Arch Clin Exp Ophthalmol. 2002 Oct;240(10):878-82.
- Augsburger JJ, Trichopoulos N, Correa ZM, Hershberger V. Isolated choroidal melanocytosis: a distinct clinical entity? Graefes Arch Clin Exp Ophthalmol 2006;244:1522–1527.
- Kovoor TA, Bahl D, Singh AD, Ufret-Vincenty R. Bilateral isolated choroidal melanocytosis. Br J Ophthalmol. 2008 Jul;92(7):892, 1008.
- Fine HF, Brue C, Eandi C, Jacobs MI, Pulitzer M, Yannuzzi LA. Bilateral isolated choroidal melanocytosis Retinal Cases and Brief Reports. 2009;3:272-273.
- Singh AD, De Potter P, Fijal BA, et al. Lifetime prevalence of uveal melanoma in white patients with oculo(dermal) melanocytosis. Ophthalmology 1998;105:195–198