West Coast Retina
Case of the Month
Dec, 2015
Presented by Kevin Patel, MD and Jill Rotruck, MD
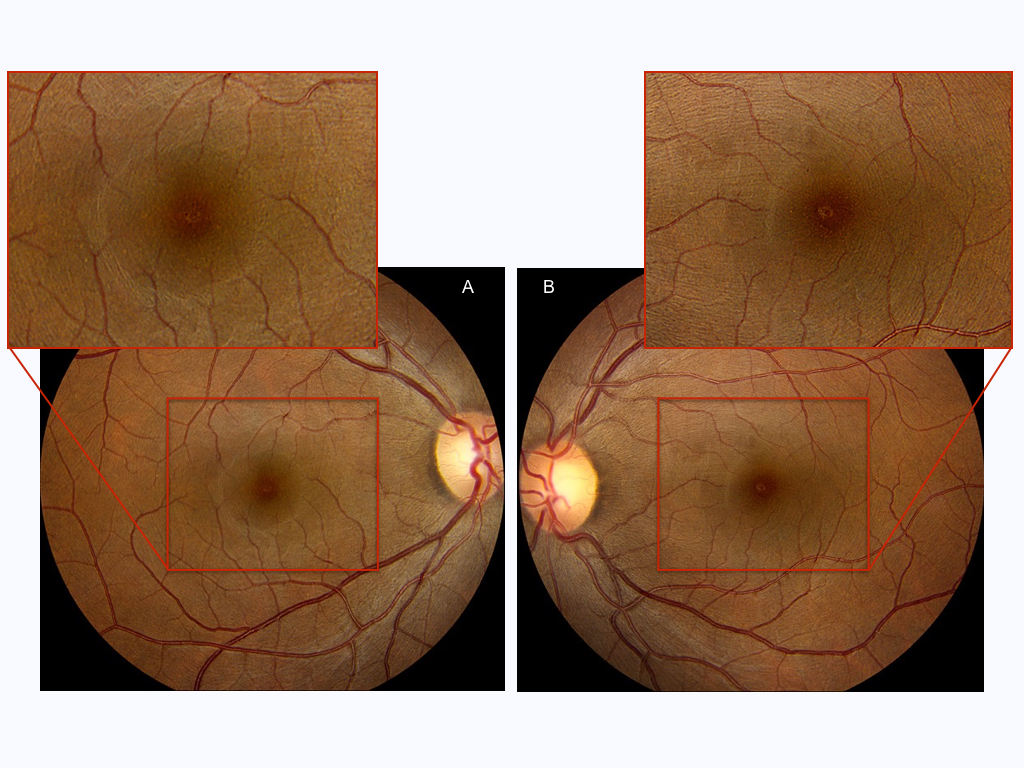
A 36 year-old Indian man presenting with blurred vision in both eyes.
Figures 1A and B: Color fundus photographs of the right (A) and left (B) eye. A small yellow spot is present at the center of the fovea in both eyes.
Case History:
A 36 year-old Indian man presented with blurred vision of both eyes that began suddenly 11 days prior to presentation. He complained of small, hazy spots in his central vision. This remained constant since its onset. The patient denied pain or any other ocular symptoms. There was no significant past ocular or medical history. Family history was also noncontributory, but his social history was remarkable for recent international travel to Amsterdam.
On examination, best-corrected visual acuity was 20/32 in the right eye and 20/25 in the left eye. Intraocular pressure and anterior segment examination were normal in both eyes. Posterior segment examination was only significant for blunted foveal reflexes with small yellow spots in the fovea bilaterally (Figures 1A and B). Fluorescein angiography was unremarkable bilaterally. Fundus autofluorescence was also normal in both eyes (Figures 2A and B). Optical coherence tomography (OCT) was remarkable for disruption of the myoid zone, ellipsoid zone, and photoreceptor outer segments in the fovea of both eyes (Figures 3A and B).
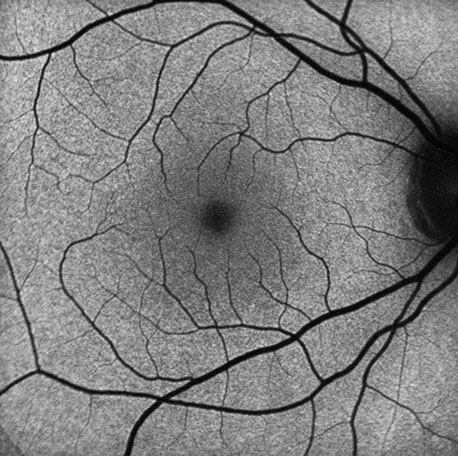
A
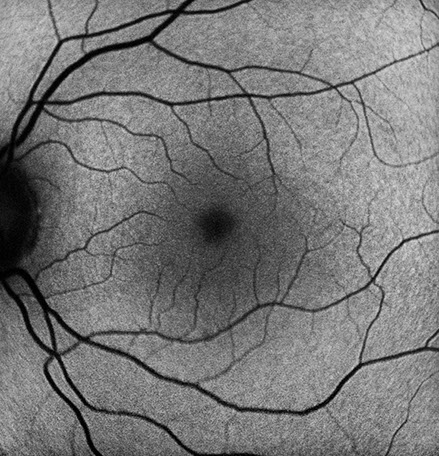
B
Figures 2A and B: Fundus autofluorescence of the right (A) and left (B) eye. Neither eye showed abnormal autofluorescence.
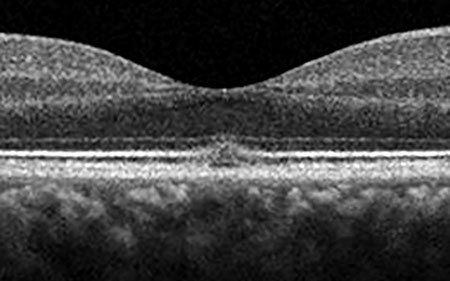
A
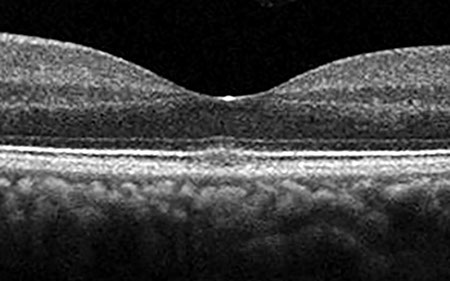
B
Figures 3A and B: Optical coherence tomography of the right (A) and left (B) eye. Note the disruption of the myoid zone, ellipsoid zone, and photoreceptor outer segments in both eyes.
Differential Diagnosis:
The differential diagnosis for small, yellow foveal lesions with outer retinal disruption includes central serous chorioretinopathy, adult onset foveomacular vitelliform dystrophy, poppers maculopathy, photic maculopathy, age-related macular degeneration, and foveal vitreomacular traction.
What is your Diagnosis?
Additional Case History:
On further questioning, the patient endorsed inhaling “poppers” with the brand name Jungle Juice while in Amsterdam on the evening prior to developing his blurred vision. This helped establish the diagnosis of poppers maculopathy. Cessation of the use of poppers and observation was recommended for the patient. His clinical course was unknown as he was lost to follow-up after his initial visit.
Discussion:
“Poppers” is a slang term referring to compounds of the alkyl nitrite family that are inhaled as recreational drugs. These substances are exogenous volatile nitric oxide donors. They are often used to induce brief periods of euphoria and can also serve as an aphrodisiac and myorelaxant. In 2006, the active ingredient in most popper brands, isobutyl nitrite, was reported to be a Class II carcinogen. This led to many brands switching their active ingredient to isopropyl nitrite.1 Since that time, multiple case of poppers maculopathy have been reported in the literature.
Several case series have described the presenting signs and symptoms of patients with poppers maculopathy. Visual acuity was only mildly affected, and patients typically complained of bilateral painless blurred vision, central scotomas, metamorphopsia, and photopsias.1-3 Posterior segment examination for most patients showed bilateral, small foveal yellow spots. The only other abnormality seen was on OCT, where there was disruption of the foveal cone outer segments and the photoreceptor inner segment/outer segment junction (or ellipsoid zone).1-3
The exact mechanism by which poppers cause foveal damage is not fully understood, but it is believed that the damage is caused by nitric oxide (NO), as alkyl nitrites are volatile NO donors.2 Nitric oxide act as a neuromodulatory molecule for the metabolism and function of photoreceptors through the activation of guanylate cyclase, which is a key enzyme involved in the recovery of photoreceptor function after phototransduction.4,5 At high doses, photoreceptors have been shown to be among the most sensitive retinal neurons to the toxic effects of NO.2 Nitric oxide is also known to decrease the threshold of light toxicity.2 Poppers maculopathy bares a strong resemblance in clinical presentation to phototoxicity.6 Audo et al hypothesized that the interaction of NO with the macular pigment zeaxanthin may impact the pigments ability to protect the fovea from light damage, potentiating light toxicity.2 Despite these hypotheses, the precise pathophysiology of poppers maculopathy remains unknown.
Due to the recency and limited number of cases reported, the natural history of poppers maculopathy is still being characterized. A majority of reported patients with follow-up had improvement in symptoms and fundus abnormalities over several weeks with a minority achieving complete resolution upon cessation of popper use.1-3
Take Home Points:
- Popper maculopathy tends to occur with poppers made from isopropyl nitrite.
- Patients typically have mild visual disturbance with foveal yellow spots and disruption of the photoreceptors on OCT. These may improve or resolve with cessation of popper use.
- While the exact pathophysiology of poppers maculopathy is unknown, a leading hypothesis suggests that nitric oxide mediates foveal damage.
References:
- Davies AJ, Kelly SP, Naylor SG, et al. Adverse ophthalmic reaction in poppers users: case series of “poppers maculopathy”. Eye. 2012;26:1479-86.
- Audo I, El Sanharawi M, Vignal-Clermont C, et al. Foveal damage in habitual poppers users. Arch Ophthalmol. 2011;129:703-8.
- Vignal-Clermont C, et al. Poppers-Associated Retinal Toxicity. N Engl J Med. 2010;363:1583-5.
- Goldstein I, Ostwald P, and Roth S. Nitric Oxide: A Review of Its Role in Retinal Function and Disease. Vision Res. 1995;36:2979-94.
- Lima M, et al. Nitric oxide as a regulatory molecule in the processing of the visual stimulus. Nitric Oxide. 2014;36:44-50.
- Fajgenbaum MAP. Is the mechanism of ‘poppers maculopathy’ photic injury? Eye. 2013;27:1420-1.