Age-Related Macular Degneration
In 1987, we began an innovative series of booklets that explain various aspects of retinal disease with easy-to-read text and graphic illustrations. Acclaimed by both patients and physicians, these booklets help patients learn about their condition and enable them to make informed decisions about their treatment.
Available through:
San Francisco Retina Foundation
1445 Bush Street
San Francisco, CA 94109
415-344-0209
The San Francisco Retina Foundation is a nonprofit organization


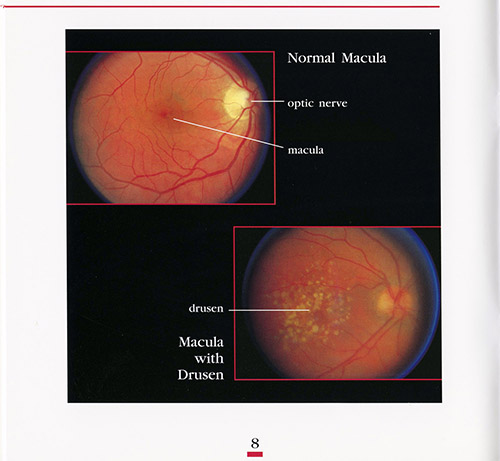
Age-related Macular Degeneration (AMD) typically occurs in people over the age of 60. Most people who have the early stages of AMD may notice little if any changes in their vision. This condition is caused by the accumulation of metabolic waste deposits under the retina, called drusen. AMD only affects the central vision, the macula (see How The Eye Works, for more details). AMD occurs in two types: dry AMD and wet AMD.
Dry AMD
The presence of the drusen can interfere with the heath of the macula and disturb the normal structure of the macula. Symptoms that people may notice is blurring of reading vision, difficulty seeing print with less contrast, difficulty with bright lights, or moving from brightly lit areas to more dimly lit areas. Over time, some dark or blank areas may occur in the vision due to weakening (atrophy) of the macula. Occasionally, dry AMD may also cause distortion of vision (bent wavy lines), though this symptom needs to be evaluated carefully for the possibility of wet AMD. It is important for all patients with AMD to contact their ophthalmologist promptly if they develop any sudden changes in their vision such as more blurring, more trouble reading, or distortion in their vision. Dry AMD may progress into wet AMD for which there are effective treatments. Testing and evaluation (see Diagnostic Testing for more details) usually involves retinal photography, fluorescein angiography and optical coherence tomography (OCT).
Wet AMD
The wet stage of AMD occurs when abnormal blood vessels grow under the macula causing leakage of serum (the clear sticky part of blood), or bleeding. These abnormal blood vessels are called choroidal neovascularization (CNV) . The leakage of these blood vessels under the macula can causing blurring of vision and distortion. Treatment as soon as possible is important.
Treatment
Over the past 10 years, there has been tremendous improvement in the treatment of wet AMD. Injection therapy is now the mainstay and has led to remarkable gains in vision and stability of vision for years.
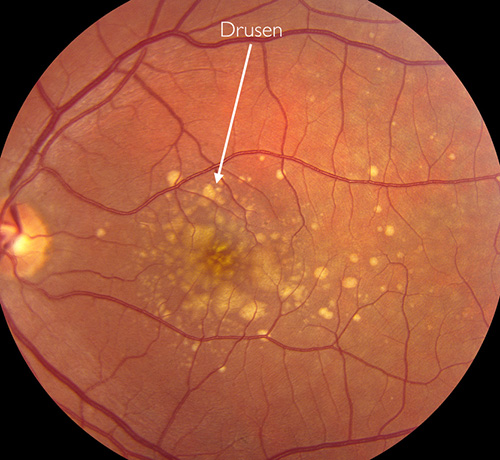
Color retinal photograph of a macula with drusen
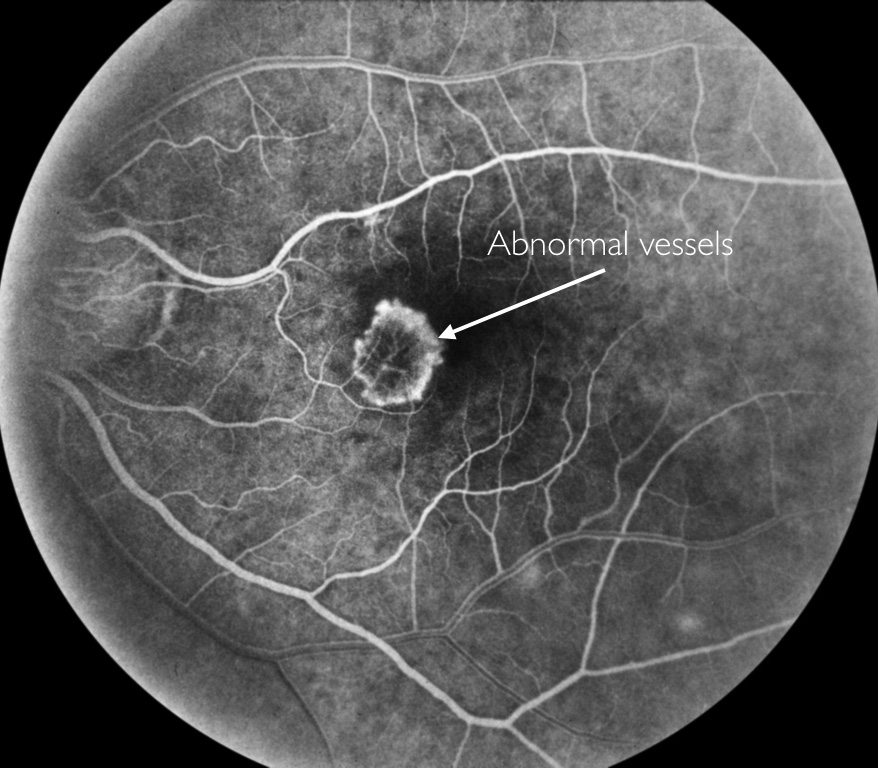
Fluorescein angiogram of choroidal neovascularization (CNV)
A protein called vascular endothelial growth factor (VEGF) is produced in our body that regulates the growth of blood vessels. In wet AMD, an excess of VEGF causes the formation of abnormal vessels (CNV). Several new drugs (Lucentis, Eylea, and Avastin) are available that inactivate the excess VEGF. These drugs need to be injected into the eye. This is called an intravitreal injection. These treatments are usually done monthly initially, and depending on how the eye responds, the treatments may be able to be done less frequently, or even paused. However, it is impossible to know ahead of time how often and how many injections any individual will need. Most patients will need continued ongoing monitoring to insure that the wet AMD is under control. While most patients initially have an aversion to the idea of an injection into the eye, numbing of the eye is carefully done, and these injections are comfortable and patients do very well.
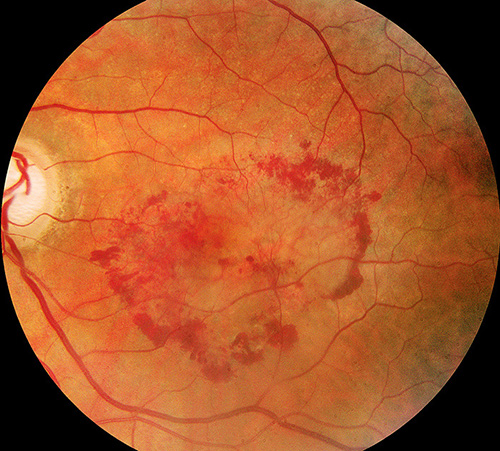
Color photograph showing bleeding in a patient with 'wet' macular degeneration. Bleeding occurs due to abnormal blood vessels, CNV, growing under the retina.
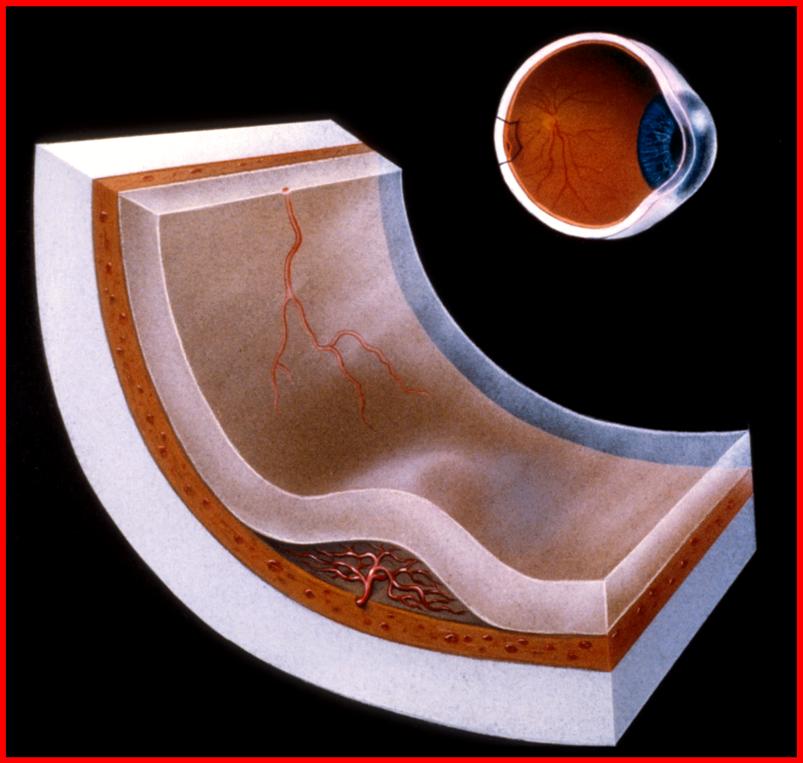
Drawing showing abnormal vessels (CNV) under the macula
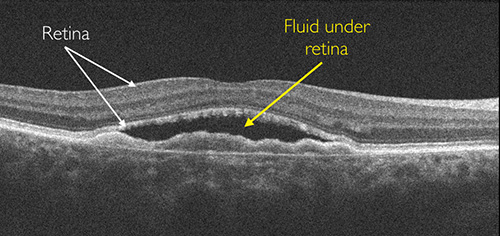
Optical Coherence Tomography showing fluid under the retina due to CNV
Other Treatments
Since intravitreal injections typically provide the best outcomes, it is less common to use other treatments. Thermal laser treatment to seal the leaky blood vessels, or a cold laser (Visudyne Photodynamic Therapy).
Thermal laser treatment to seal leaky blood vessels causes damage to the tissue, and therefore it is usually used when the CNV is further away from the center of vision.
Photodynamic treatment uses a drug, Visudyne, that is infused in a vein. This drug is absorbed by the CNV. A laser light is used to activate the drug which causes the blood vessels to close and stop leaking without the same type of damage that thermal laser treatment causes.
Health Factors and Nutrition
Risk factors for AMD include age, smoking, high blood pressure, family history of AMD, heart disease, elevated serum lipids and an increased exposure to bright sunlight. Managing your health is an important adjunct to the treatment of your eyes and AMD.
Vitamins (Antioxidant Supplements)
Several important studies (Age-Related Eye Disease Study, AREDS) conducted by the National Eye Institute have demonstrated that supplements of the antioxidants lutein and zeaxanthin and zinc are helpful to slow the progression of AMD. These supplements can be found in your local pharmacy. You should discuss with your doctor the advisability of taking these supplements based on the status of your eyes.
Monitoring Your Vision
It is very important for patients with AMD to self-test their eyesight regularly, at least weekly. When testing, it is important to test EACH eye separately. It is not uncommon for AMD to progress in one eye undetected unless each eye is tested. Traditionally, patients have been instructed to use an Amsler Grid chart to test their vision. A copy can be downloaded below with instructions on its use. We also ask our patients to test their reading vision in each eye as well as our experience has shown that sometimes patients may overlook, or not see, abnormalities on an Amsler Grid, even though they have noted a worsening of their reading vision. If their is a definite change in either your reading vision or Amsler Grid testing, then it is important to contact your eye doctor promptly for evaluation. You should not wait for your next scheduled appointment to be seen.

